Have you been noticing some strange symptoms in your thigh? If numbness, tingling and pain have you concerned, it could be meralgia paresthetica.
Although you may have never even heard of the name of this condition, the sensations it causes are not easy to forget – something you’ll know if you’ve experienced its odd, painful symptoms.
But with a few strategies I’ll show you today, you could soon be saying adios to these uncomfortable sensations.
Strange Sensations… Or a Lack Thereof
Imagine this.
You’ve just come off a shift at work, where you’re standing on your feet for hours.
You noticed a strange tingling along your upper outer thigh at work, but it was mostly just annoying, and you were busy, so ignored it.
But later that night, as you tried to fall asleep, the sensation became much more difficult to ignore. The tingling intensified until it felt like the skin on your thigh was burning, and every shift of the sheets over your leg hurt like hell.
This continues for several weeks, with the tingling and burning coming and going – especially after a long day at work.
But then things get really strange. You start to notice the same region of your thigh is almost… numb.
One Sunday morning, you’re curled up with a book and a piping hot cup of coffee…
As you shift yourself on the couch to get comfy, you spill the good stuff right on your leg.
The thing is, you didn’t feel the hot coffee on your leg.
You stare down at the strangely painless red welt on your now coffee-covered leg and think it might be time to figure out what is causing these strange symptoms in your thigh.
What is Meralgia Paresthetica?
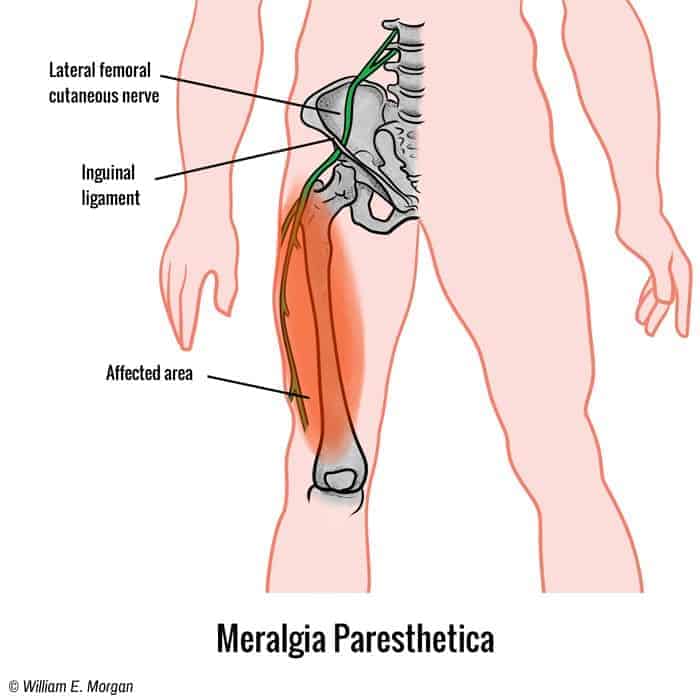
Meralgia paresthetica, also called lateral femoral nerve entrapment, is a condition that appears when a major sensory nerve in your leg, the lateral femoral cutaneous nerve (LFCN), is compressed.
Your LFCN runs from the spinal cord to the pelvis and thighs to innervate your hip flexors and leg extensors [1], plus allow for feeling in the anterolateral (front and outside) regions of your thigh.
Because this nerve is strictly SENSORY, and not a MOTOR nerve, the compression does not affect the way you move your muscles [2].
It does, however, affect sensation in the region, and its effects can be quite unpleasant.
Common Symptoms
The symptoms of meralgia paresthetica can vary in sensation, but they all show up in the same region of your leg – the front and lateral region of the thigh, or the area innervated by your LFCN.
In this area, meralgia paresthetica can cause a painful burning feeling for some. For others, it can cause an uncomfortable tingling, “buzzing” sensation that some have likened to a phantom ringing cell phone [3].
And for some, it can cause numbness in this region of the leg.
For many, the condition also causes a great sensitivity to light touch – more so even than harder pressure [4].
These symptoms might feel worse after time spent on your feet, whether that’s standing at work or going on a long walk [5]. This may be because the tension on the LFCN is reduced when sitting, thereby alleviating symptoms in the process [6].
What’s Causing Compression?
We’ve learned that compression of the LFCN is behind these sensations, but what is going on to cause the compression?
There are two potential sources of compression; (1) internal compression from the muscles, fascia, and fat or (2) external compression can occur from exterior sources from clothing, such as a trouser belt, or weight belt. Look for any external sources of compression to the LFCN. The fix is simple here, adjust the positioning of the belt and your symptoms should resolve.
In many cases, the LFCN is being internally compressed between two structures inside the pelvic region, the anterior superior iliac spine (ASIS) of the pelvis and the inguinal ligament.
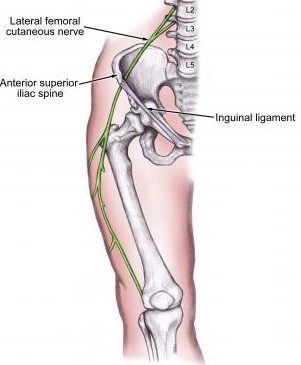
Your ASIS is a bony protrusion at the front and top of the pelvis – this is that bony bump you can feel at the front of your hip.
Your inguinal ligament runs from the ASIS to the pubic tubercle at the front, lower region of the pelvis [7].
The LFCN passes through a narrow region between these two structures. If something changes, like say an increase of swelling or pressure, the nerve can easily become compressed.
Factors like hip injuries and repetitive leg motion (like perhaps those required in running) have been tied to meralgia paresthetica [8]. It’s not hard to imagine how inflammation or tightness from these factors could reduce space for the nerve.
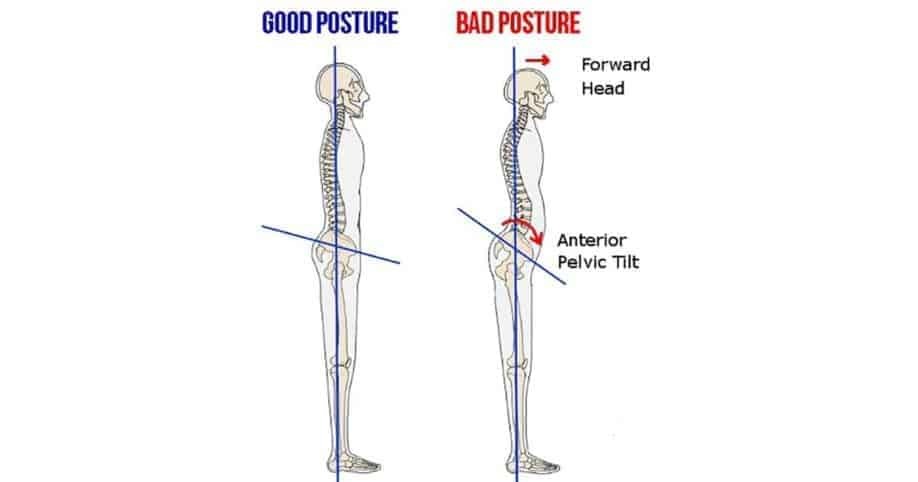
For other patients, anterior pelvic tilt may be related to meralgia paresthetica.
This improper pelvic positioning is associated with tightness in many muscles along the front of the pelvis and hips. This increased tightness could contribute to unnecessary pressure on the LFCN.
To learn more about this postural dysfunction, including a 6 minute routine that will help you tackle it, check out my article on anterior pelvic tilt.
Do I need special tests to make the diagnosis of Meralgia Paresthetica?
Generally your doctor can make the diagnosis with a good history and physical examination. The most common physical examination findings are numbness in the LFCN distribution. Occasionally, lightly tapping the nerve where it exits the abdominal cavity, just under the inguinal ligament may cause a tingling sensation known as a Tinel’s sign. Other causes of pain and numbness in the thigh such as degenerative disc disease of the lumbar spine can be ruled out by your doctor. Very rarely a nerve conduction study is required to make the diagnosis.
Meralgia Paresthetica Treatment Strategies
Most people with Meralgia Paresthetica get better once the compression on the nerve is reduced. It may take several months for normal sensation to return, but the pain settles down quickly once you address the reason for the nerve compression. Treating femoral nerve entrapment requires incorporating several different approaches – the 4 R’s (check out my article on the 4 R’s).
- Relax the surrounding tissues through soft tissue work
- Restore- improve hip mobility
- Reset
- Reprogram pelvic stabilization through core exercises
The key to effective treatment of LFCN entrapment is to fix the underlying movement issue that has created the tight tissues around the nerve. We do this by restoring our foundation for movement with the 4R’s.
Before we get into the 4 R’s you may be wondering about other interventions or if surgery is ever needed to treat MP? It is extremely rare! Due to the fact that there are so few cases requiring surgery it makes it difficult to really understand the effectiveness of other treatment strategies.
There is some evidence that an injection of local anaesthetic and steroid can help those who do not respond to the 4 R’s or have an underlying metabolic issue, but a simple injection will not correct the primary cause of the nerve compression.
Surgery, if performed, would involve resecting or burning a part of the nerve in an attempt to prevent the pain impulse from propagating along the nerve. There are so few studies it is really hard to say how effective this surgery is, I would recommend doing everything else besides surgery in this case as your chance of recovery is high.
If you do have surgery remember that you will be left with a patch of numbness on your thigh forever.
In my clinical experience the 4 R’s will more than do the trick, as it will address the underlying root issue as to why the LCN is being compressed, which injections or surgery do not.
So let’s get started!
1. Relax – Soft Tissue Treatment
Release fibrotic connections between the surrounding muscles and fascia so that they are not compressing the nerve. ASMR promotes sliding and natural movement of the nerve along its anatomical path.
Foam Rolling the Quads
This Active Self-Myofascial Release (ASMR) technique helps create shearing forces that can increase the length of tissues while releasing fascia and trigger points in the quadriceps.
This technique also takes advantage of reciprocal inhibition – when you contract your hamstring, your quad relaxes. By actively contracting your hamstring, you’re better able to relax the quads, getting deeper into the tissue to release tension more effectively.
- Lay prone with a foam roller underneath one quad and your upper body propped up on your forearms
- Start by rolling back and forth on the foam roller, from just above the knee to the hips
- When you hit a painful point, pause and relax over it
- Press your weight into the roller and rock side to side over that area
- After a moment, start to move on the roller again, stopping and working into any trigger points you encounter
- Now, start with the roller at your knee and your weight into the roller
- Begin to roll up towards your hip, bringing your heel towards your butt as you go
- When you get to your hip, return to the start and repeat
- Repeat the entire process on your other leg
Lacrosse Ball SMR for Psoas
This is another self-myofascial release move that is great for getting rid of adhesions and fascial restrictions in the psoas. It will also help to lengthen the tissue in the process.
All this together allows for increased flexibility and mobility, reducing the likelihood of compression.
- Start by locating your hip bone – the ridge you feel along the side of your pelvis
- Follow the ridge in towards the midline, stopping about an inch from your belly button – this is where you’ll want to start with a lacrosse ball
- Lay supine and place a lacrosse ball at this spot
- Now hold a dumbbell on top of the ball, bending the on that side knee and placing the foot on the ground for support.
- Relax and breathe, pressing the dumbbell into the ball
- After a moment, exhale as you slowly slide your foot back out until your leg is long
- Inhale as you bend the knee to bring the foot back in, repeating 3-5 times
- Remove the dumbbell and move the ball about an inch lower, repeating the entire process
- Repeat once more after moving ball another inch lower, then switch sides!
Transverse Friction Massage of the Inguinal Ligament
This technique will help encourage release of the inguinal ligament. Doing so will help reduce tension in the region and LFCN compression.
- Lay supine and locate your ASIS by feeling for the bony protrusion at the front of your hip
- Next locate your pubic symphysis – the broader bony region at the front of your pelvis
- The inguinal ligament will run between these two landmarks, so use these as your guide
- With your fingers, press down between the ASIS and pubic symphysis, moving back and forth to release the tissue
2. Restore Hip Mobility
It is critical to restore normal range of motion so that the soft tissues are balanced and the muscles can work throughout their normal excursion. When muscles are too tight or imbalanced, they can pinch the LFCN.
DCR Hip Flexor Stretch
This Dual Contract Relax (DCR) approach stretches the hip flexors while also building strength.
The psoas and glute will be activated as you extend and reach the end range of motion – a much more effective approach than a passive stretch requiring little activation.
- Take a kneeling lunge position on the ground with your front leg at a 90° angle in front of you
- Attach a band at about knee height and loop the other end of the band around your kneeling leg just under your butt
- Slightly lean forward so that your hip on the side of you kneeling leg is in extension
- Make sure you maintain good neutral posture, chin tucked and shoulders retracted back and down throughout this exercise
- In this extended hip position, imagine you’re going to drag your knee forward without actually doing it. This will activate the psoas of the kneeling leg while at the same time activating the glute of your other leg. Hold this activation for 10 seconds
- Relax in the extended position and feel the stretch for 10 seconds
- Now, squeeze the glute on the kneeling leg and use that squeeze to drive your hip forward into the extension
- Focus and squeeze your glutes as tight as possible for 10 seconds
- Relax your glute and hold the extended position for 10 seconds
- Repeat 2 times per side
Supine Hip PNF
This next drill is a proprioceptive neuromuscular facilitation (PNF) approach.
This move will work hip mobility – and hip CONTROL – throughout a huge range of motion.
- Lie supine and lift your right leg while internally rotating the foot
- Extend the leg to your left, moving through your full range of motion
- From there, move your leg up and around in a circular motion, bringing your leg down and extended on the right side of your body
- Repeat, moving through your full range in every direction and maintain extension through your leg
- Switch directions, rotating the leg and hip externally to activate and stretch the entire hip
3. Reset – Pelvic stabilization/abdominal core exercises
Engaging the proper muscles in the pelvis and core will help to ensure that the soft tissues compressing the nerve maintain their proper length preventing a recurrence of nerve compression.
Glute Bridges
Utilizing glute bridges will activate and strengthen the glutes, which provide a lot of stability to the spine and the entire pelvic region.
As you’re executing this move, stay conscious about squeezing the glutes actively with each rep.
- Lay supine with knees bent and feet planted on the floor
- Squeeze your glutes in this starting position to begin activation
- Continue squeezing as you press into the heels to lift your hips up
- Hold for two counts at the top, then release down
- Repeat, completing 10-12 reps
4 Point Opposites aka Birddog
This drill is great for building strength and stability throughout the entire core.
It doesn’t just help those abdominal muscles along the anterior of your body, it also helps your lower back muscles, improving stability along the posterior as well.
It will also work pelvic alignment as you build strength while balancing through one side of the hips.
- Taka a quadruped stance on the ground with your hands shoulder-width apart and your knees and feet at hip width
- Retract the shoulder blades back and down
- Rotate the elbows inwards to create stabilizing tension in the lats
- Maintain a neutral spine while keeping your chin tucked
- Slowly lift one leg and stretch it behind you making sure not to rotate at the hips
- Now, slowly raise your opposite arm, thumb up, at a 45-degree angle from your head and hold for 10 seconds
- Breathe naturally, making sure there is no rotation left or right of the hips, shoulders or the core
- Slowly return your hand and knee to floor
This combination of soft tissue techniques, hip mobility work and pelvic and abdominal stability drills will go a long way toward addressing the uncomfortable symptoms of meralgia paresthetica.
Increased mobility, whether through more traditional exercises or soft tissue techniques, means that tissues are freer to move, with less chance for compression and impingement.
And stabilization of the pelvis helps you solidify and maintain proper form, muscle engagement and alignment, further reducing the chance of femoral nerve entrapment.
Give these moves a go and you’ll probably soon be saying, “SEE YA!” to the strange tingling, burning and numbness in your anterolateral thigh.
I’m sure you won’t be sad to see them go.